1 min read
3 Important Current Events in Veterinary Medicine
Staying on top of everything going on in the industry can be tough, so we'll help by filling you in on some hot topics—the One Health Initiative,...

There hasn't been a better time for veterinarians and human healthcare providers to come together and discuss how to keep families safe from zoonotic diseases.
In the wake of a pandemic caused by a disease jumping from animals to humans, it is more important than ever that the general population has a better understanding of zoonotic diseases and that veterinary medicine and human medicine are on the same page.
In a recent Facebook live event, we brought together a veterinarian who works in public health as an associate professor of One Health epidemiology, Dr. Audrey Ruple, and an associate professor and practicing physician of clinical pediatrics at Weill Cornell Medical’s Division of Infectious Diseases, Dr. Patricia DeLaMora.
These two specialists answer questions about how to lower the risks of a zoonotic disease infecting family members, human or animal. They also discuss cases where there could be more communication between veterinarians and human medical professionals in cases of zoonotic disease diagnosis.
While we’re all familiar with the most common zoonotic diseases in animals and humans including salmonella infections, Lyme disease, and others, there are some reemerging ones that we should also look out for.
Both Dr. Ruple and Dr. DeLaMora mentioned toxoplasmosis being a concern in correlation with pregnant women (and felines). We don’t see a lot of cases—Dr. DeLaMora does treat infants whose mothers were infected—but it’s important because of the potential negative outcomes.
One reemerging disease we’re seeing in dog populations, believe it or not, is rabies! That’s one reason helping animals and people get the proper vaccines is an essential part of medical professionals’ role in public health.
When asked about possible exposures to avoid, here are some things that both doctors recommended:
General populations don’t understand zoonotic diseases, and educating patients and clients is a vital role that public health professionals play. Veterinary professionals, when diagnosing a patient with a zoonotic disease, can take the time to explain to the client that this diagnosis could affect them and their household, especially if there is someone who is immunocompromised.
A topic that should always come up when talking to clients about zoonotic disease is the prevalence of ticks. Due to climate change, there is practically no more “tick season”—it’s year-round now.
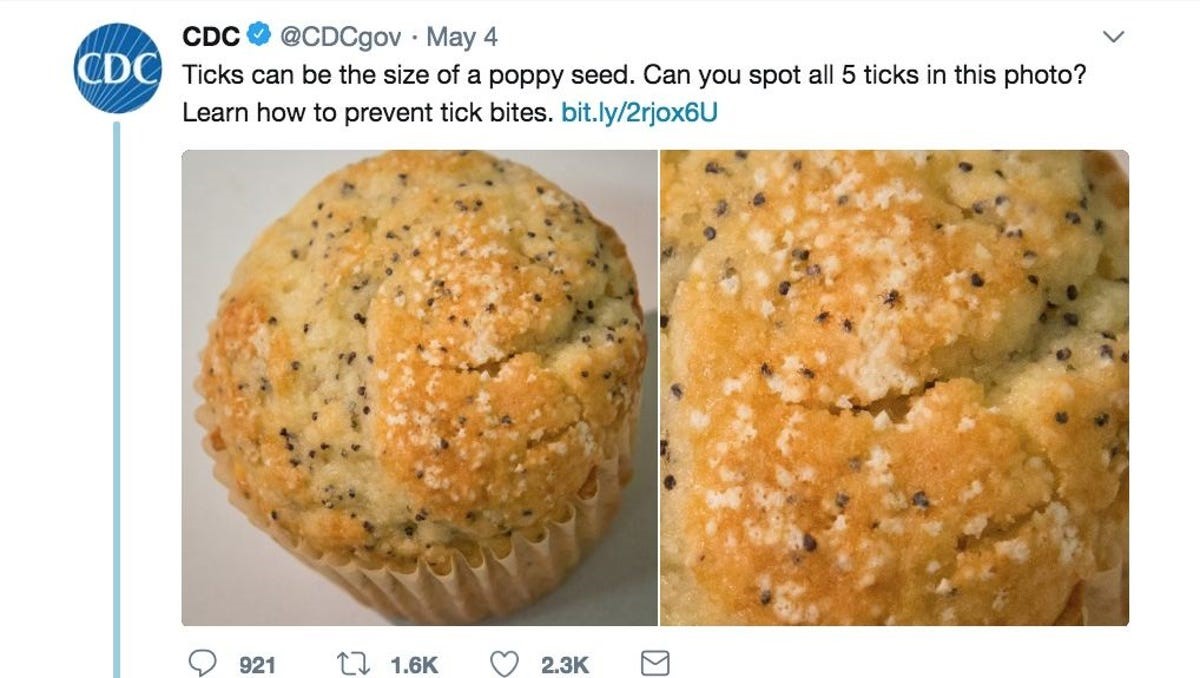
If someone needs to be scared into being careful while walking through tall grass and checking themselves and their kids for ticks, you can show them the horrifying photo the CDC took when they put tiny ticks on a poppy seed muffin. Ticks are small!
In some good news for veterinarians, Dr. Ruple says that a study found that 90% of clients are willing to consider their veterinarian part of their own healthcare. This inclusion means that clients are likely to be open to having their veterinarians reach out to their family physicians in the case of a zoonotic disease confirmation.
As an infectious disease specialist, Dr. DeLaMora has had people bring veterinary records for their animals to her for answers about how it affects their family and kids. Interestingly, many spring breaks and summers bring phone calls from parents worried about their kid vacationing in Madagascar who said they’d been nibbled by monkeys there. Dr. DeLaMora was able to talk with the veterinarians working with the primates to reassure parents that the monkeys were healthy and vaccinated.
This kind of communication isn’t just helpful, but it should happen more often. When a veterinarian confirms the presence of a zoonotic disease, that veterinarian should feel comfortable reaching out to the family’s physicians. Dr. DeLaMora indicated that the more information and cooperation, the better.
The furthering of the One Health initiative—combining the efforts of veterinary, human medical, and environmental professionals around the world—is exciting as we continue to have discussions like this one. In the process, we remember the public oath we took to protect the health of everyone, animals and humans alike. Veterinary professionals are empowered to make a bigger difference, and it reinforces the veterinarian’s role in public health, especially as relates to zoonotic disease.
Visit Viticus Group's COVID-19 in Veterinary Practice webpage to get more news, updates, resources, and blogs about this novel virus.
Subscribe to our YouTube channel or check out our Resource Library full of great podcasts, videos, and digital downloads!
Disclaimer
Content may contain advertising and sponsorships. Advertisers and sponsors are responsible for ensuring that material submitted for inclusion is accurate and complies with applicable laws. We are not responsible for the illegality of any error, inaccuracy, or problem in the advertiser’s or sponsor’s materials.
Advertising material and/or opinions are not are not a reflection on Viticus Group.

1 min read
Staying on top of everything going on in the industry can be tough, so we'll help by filling you in on some hot topics—the One Health Initiative,...
1 min read
On March 23, eleven veterinary leaders gathered and collaborated during an online summit organized by Viticus Group to inform the veterinary...

1 min read
We all have a story—decisions, motivations, experiences, and maybe a little bit of luck that makes us who we are. As the veterinary class of 2022...