1 min read
Live Stream Surgical CME Training for the Win
When it comes to learning surgical techniques, hands-on experience is the way to go. When that's not possible (during a pandemic), watching another...
5 min read
Megan Skeffington, DVM, CCFP : October 14, 2020 8:00:00 AM PDT
.jpg)
My surgical abilities may have been rooted at Iowa State University, but my skillset blossomed through practice and attending hands-on surgical lab courses such as at the WVC Academy.
.jpg?width=640&name=Megan%20(14%20of%2017).jpg)
It was a typical Tuesday morning at the hospital. The normal sounds of the treatment room filled the air. Phones were ringing, patient arrival announcements were crackling through the intercom, the humming of a centrifuge muted nearby conversations of techs and assistants, and as always, some IV pump was chirping “air in line” through the mumbles of a technician pleading with the perfectly air-free fluid line.
In the back of the surgery suite where I was standing, the familiar beeps of the ECG and pulse oximeter kept time like a metronome. Wires and tubes crisscrossed between the patient and the monitoring equipment. The buzz of the blood pressure cuff gently filling then clicking away as it took its reading until the final “sigh” it takes as it decompresses, displaying numbers that made my newly trained technician very pleased.
The surgeon, a young vet that was here today learning how to do an incisional gastropexy with a spay on his Great Dane patient was focused and just had begun to explore the abdomen. A small bead of sweat was visible on his brow between his cap and his mask. This chaotic yet comforting scene and the song of a busy hospital was music to this chief of staff’s ears.
About two minutes later, a now very nervous voice rang out an unexpected lyric that filled the room. “Dr. Skeffington, I can’t find the stomach.”
“Come again?” I inquired, as surely, I must have misheard. “I know she’s deep chested, but I searched everywhere, and I cannot find the stomach.”
“Ok,” I said. “Let’s retrace our steps and start with finding a section of small intestine and work your way through that.” As a surgery coach, I’m not one to jump right in unless the patient is in danger. I am a believer that confidence comes from doing. Roughly 30 seconds later, the surgeon’s hands completely paused, his head slowly looked up and his dilated pupils locked with mine. His voice was now clearly shaking. “I…I…I think I am touching the heart.”
I swallowed hard. I first glanced toward my technician who had become quite pale in the face, then rapidly looked at all the monitors. All was good with the numbers. I ask my tech, “All good on your end?” She gave me a slow yet confident nod. “Ok, good! I’m going to scrub in and help investigate. No worries, guys, we will figure it out. Keep her steady.”
As you can imagine, a flood of thoughts went through my head as I was scrubbing, gowning, and gloving in. I pushed my way through the door, gloved hands in the air, and walked to the table. The surgeon was well over 6 feet tall, and our Great Dane at just over a year old was almost full-grown herself. At just shy of 5’4, I needed a milk crate step stool to fully visualize the deep abdomen of this girl.
As I looked and felt around, sure enough, it was what I had begrudgingly dreaded. This patient had a congenital communication between the pericardial and peritoneal spaces, known as a peritoneal-pericardial diaphragmatic hernia (PPDH). I had read about it in school, and of course, this is very rare.
Now, I was incredibly fortunate to have been trained at Iowa State University by, in my opinion, some of the best veterinary surgeons in the country at the time. These surgeons not only taught us technical skills, but they taught us the confidence we needed to calmly and comfortably address any complication we may come across during a procedure.
How did they do it? In the words of Dr. David Merkley, the head of the surgical department, they provided us an opportunity to “get to the table” as often as we could. Dr. Merkley assured us that the more times we were able to handle tissue, practice techniques, predict possible complications, and get comfortable with how we would handle the unexpected, the more robust our toolbox would be to confidently handle any surgical situation.
Throughout our 3rd and 4th years, the surgery program and externships with shelter medicine allowed me to clock in well over 100 spays or neuters and several splenectomies, cystotomies, gastrotomies, enterotomies, gastropexies, and so on. “Getting to the table” prepared me for this moment.
After making my diagnosis, several things had to fall into place to decide our next steps. I calmly shared my findings with the team and asked the other doctor to start going over manual ventilation techniques with our technician in the event we needed them. I was not blessed to have a ventilator in general practice. I needed to get the owners on the phone.
My conversation with the owners recommended this case be referred to a specialist, as correction of these conditions can be quite complex, and post-op supportive care while the patient adjusts to the newly divided spaces should be 24/7, especially with a newly reconstructed thoracic cavity. Unfortunately, due to finances, this option was off the table. The owners had worked for some time to save up funds for the spay and pexy alone. The owners were considering euthanasia.
I couldn’t let that happen. Although I had never, and probably will never again, see this condition, I knew I had the skill to attempt the repair. Through careful, thoughtful, and calm words, I had a colleague get on the phone with me and we talked through options with the clients. We would proceed with the repair attempt at no charge, knowing this was the alternative to euthanasia or closing her up and giving her a shortened life span. The owners were aware of the risks, and they were incredibly grateful I was willing to try.
“Ok team, we are doing this.” I had repaired diaphragmatic hernias before, I had done a pericardiectomy, I had done plenty of gastropexies and I had tapped air off of many chests with a 3-way stopcock and a 60cc syringe—just not all at the same time. I pulled out the trusty old green Fossum’s Small Animal Surgery 2nd Edition and had it open on a stool to my right, so I could glance at the open pages 798-800. A little PPDH PTSD you ask? Definitely.
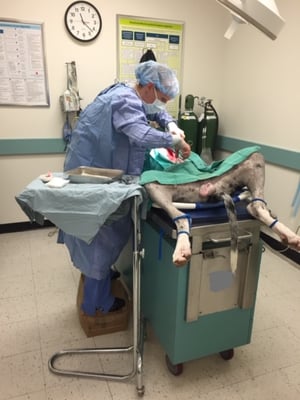
I won’t bore you with the surgical steps taken, the peeling of the liver off the myocardium, the reconstruction of the diaphragm under manual ventilation, the spay, the pexy, the intra-op radiographs to determine how much air was left to remove from the chest to achieve negative pressure, or the suspected size of the adrenal glands of all of the team members in the room that day. But what I will tell you is that the procedure was a success. Our patient did phenomenally and lived several years after the procedure, passing from an unrelated condition.
What happened that day will remain imprinted in the memories of all involved. When I’ve seen these colleagues at events over the years, we all immediately go back to the minutes of that day. Everyone in that room was navigating unfamiliar waters, but I know my success was attributed to having a phenomenal team at my side and my experience of “getting to the table.”
My surgical abilities may have been rooted at Iowa State University, but my skillset blossomed through practice and attending hands-on surgical lab courses such as at the WVC Academy. Although will we never be prepared for every possible scenario we will encounter in our career, choosing to take advantage of every opportunity to practice surgical techniques and build confidence just may be life-saving to that next patient that needs you.
Pull up a milk crate, and get to the table.
Check out the new courses coming up in 2020 WVC Academy, taught by experts in state-of-the-art lab facilities!
Content may contain advertising and sponsorships. Advertisers and sponsors are responsible for ensuring that material submitted for inclusion is accurate and complies with applicable laws. We are not responsible for the illegality of any error, inaccuracy, or problem in the advertiser’s or sponsor’s materials.
Advertising material and/or opinions are not a reflection on Viticus Group.
1 min read
When it comes to learning surgical techniques, hands-on experience is the way to go. When that's not possible (during a pandemic), watching another...

1 min read
Hands-on continuing education can play a significant role in distributing updated knowledge to medical professionals, helping narrow the...

1 min read
Despite all the challenges facing hands-on medical training in 2020, WVC Academy at the Viticus Center looks forward to hosting soft tissue surgery...